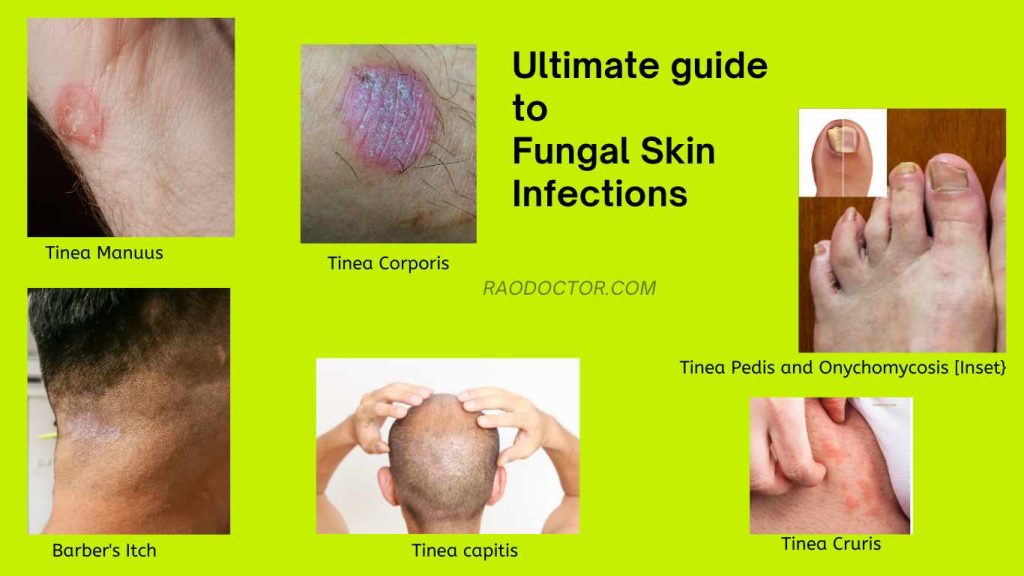
Understanding Black Skin Fungal Skin: Causes, Diagnosis, and Treatment
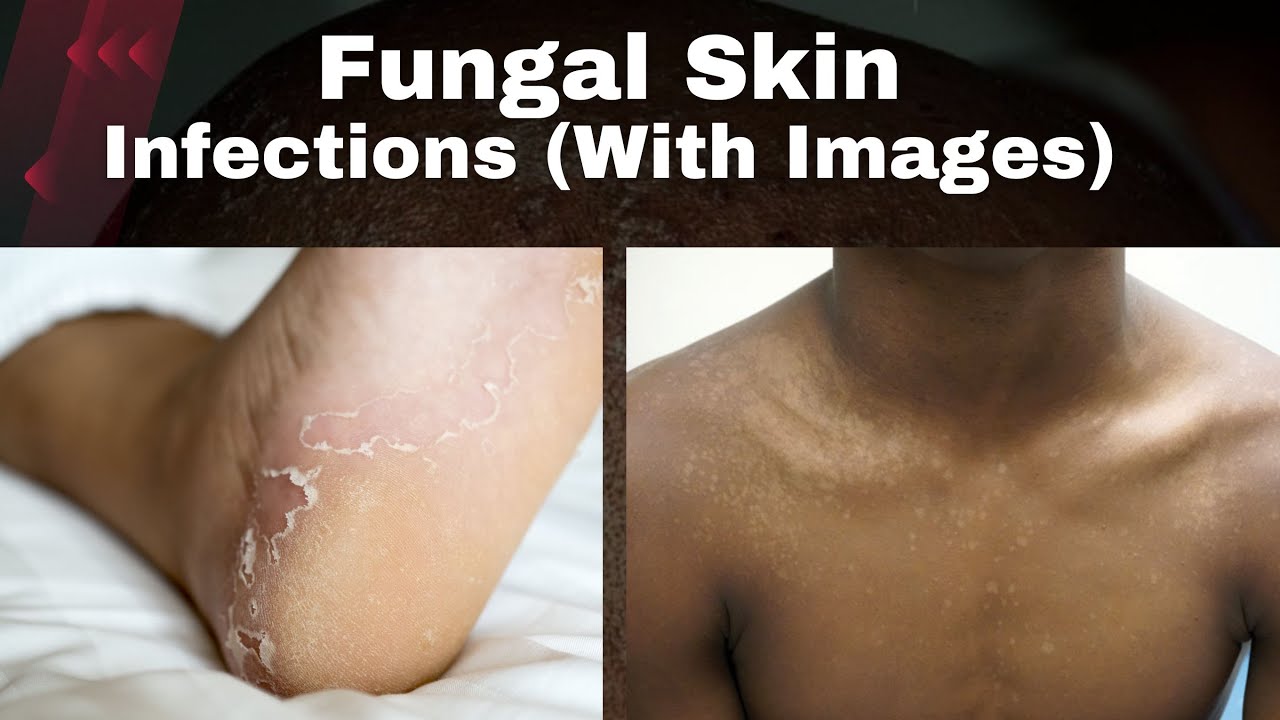
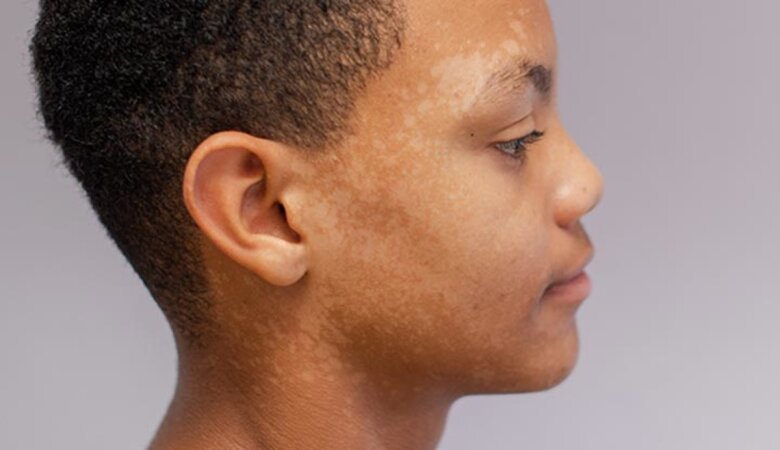
Fungal skin infections are common and can affect anyone, regardless of their skin type or ethnicity. However, people with black skin may be more prone to fungal infections due to various factors such as skin pigmentation, humidity, and exposure to certain environments. In this article, we will discuss the causes, diagnosis, and treatment of black skin fungal skin, including prevention tips and remedies to maintain healthy, clear skin.
What is Black Skin Fungal Skin?
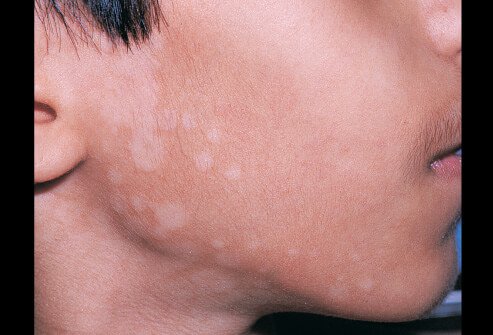
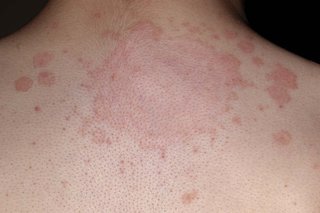
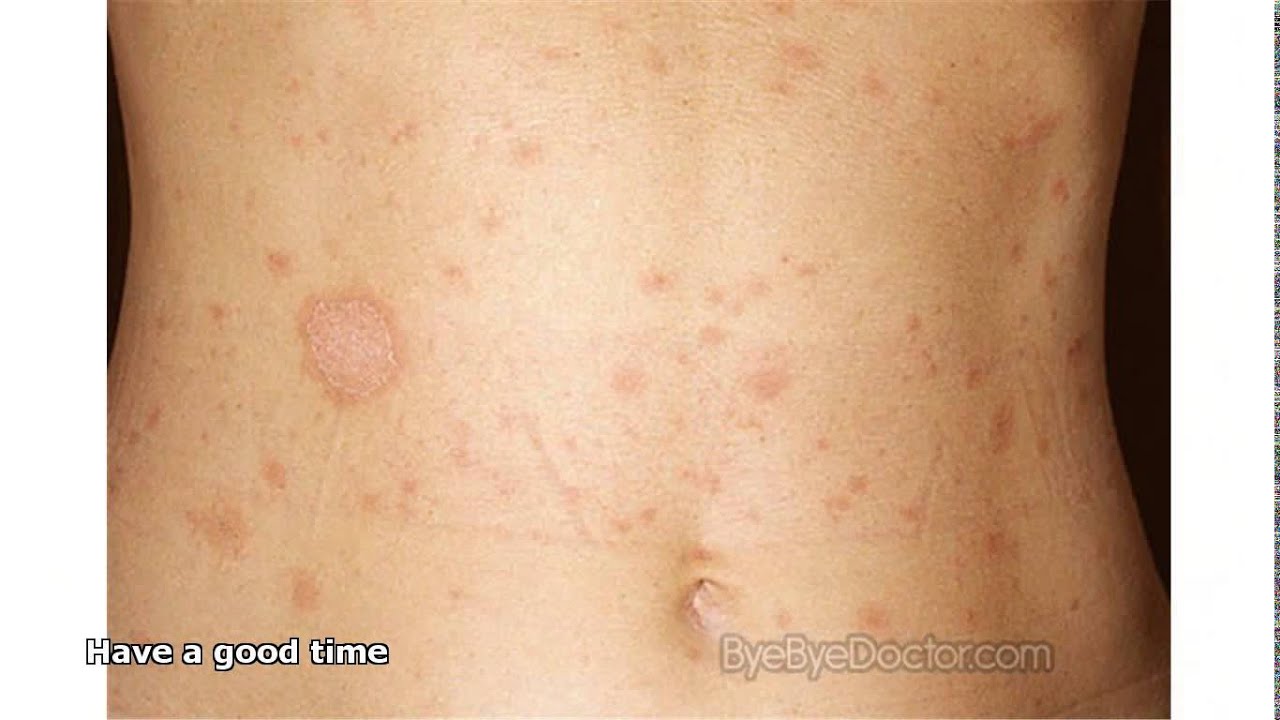
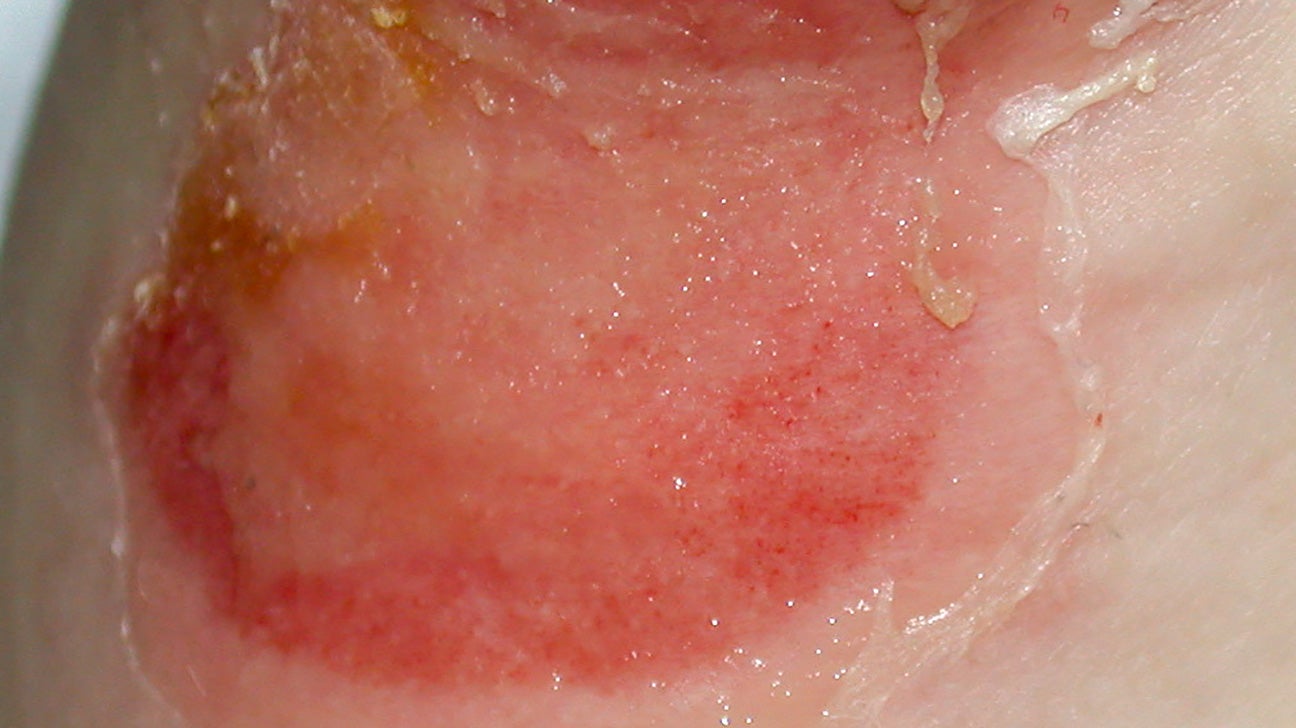
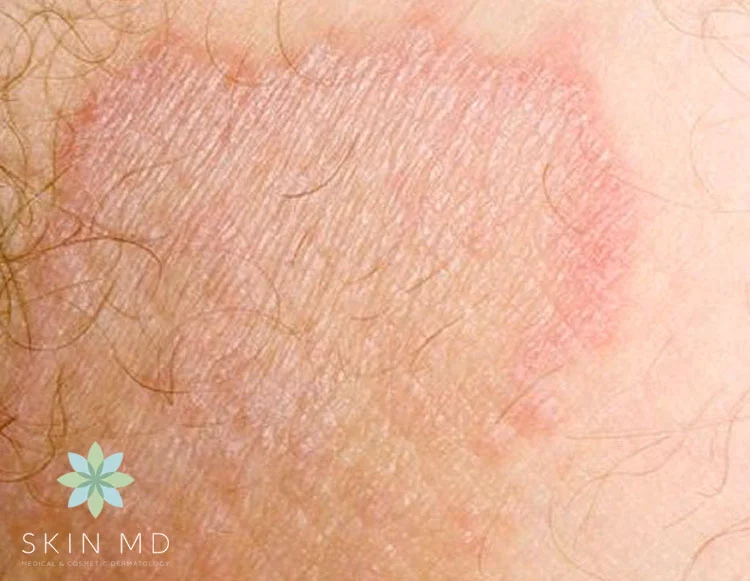
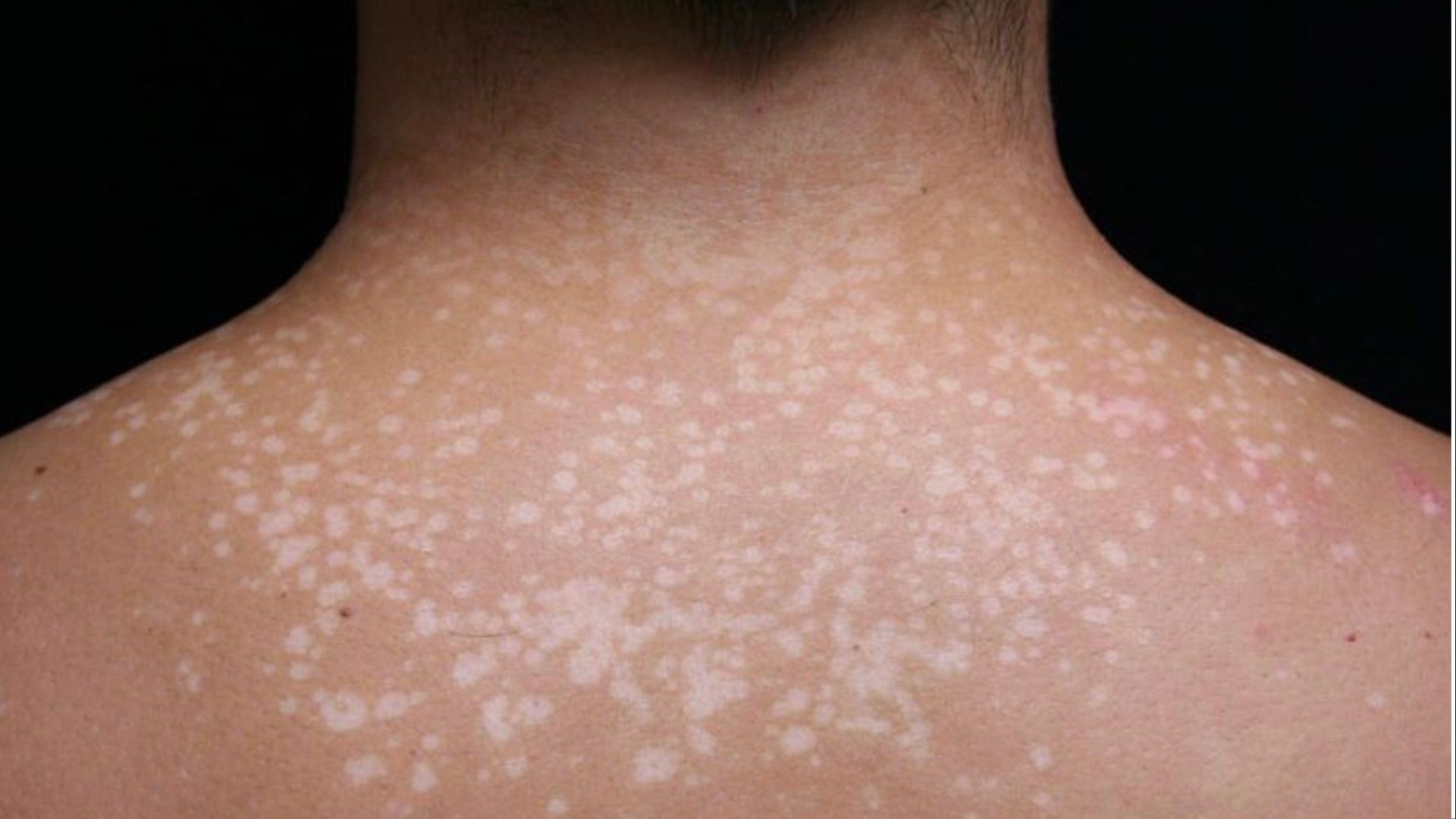
Black skin fungal skin, also known as mucormycosis, is a rare but potentially life-threatening fungal infection caused by a group of fungi referred to as 'mucormycetes'. These fungi are found in the environment, particularly in compost, animal dung, soil, leaves, and decaying organic matter. When these fungi come into contact with the skin, they can cause an infection, leading to symptoms such as redness, irritation, itching, and scaly patches.
Causes of Black Skin Fungal Skin
:max_bytes(150000):strip_icc()/GettyImages-583679466-57ac80c93df78cf459929196.jpg)
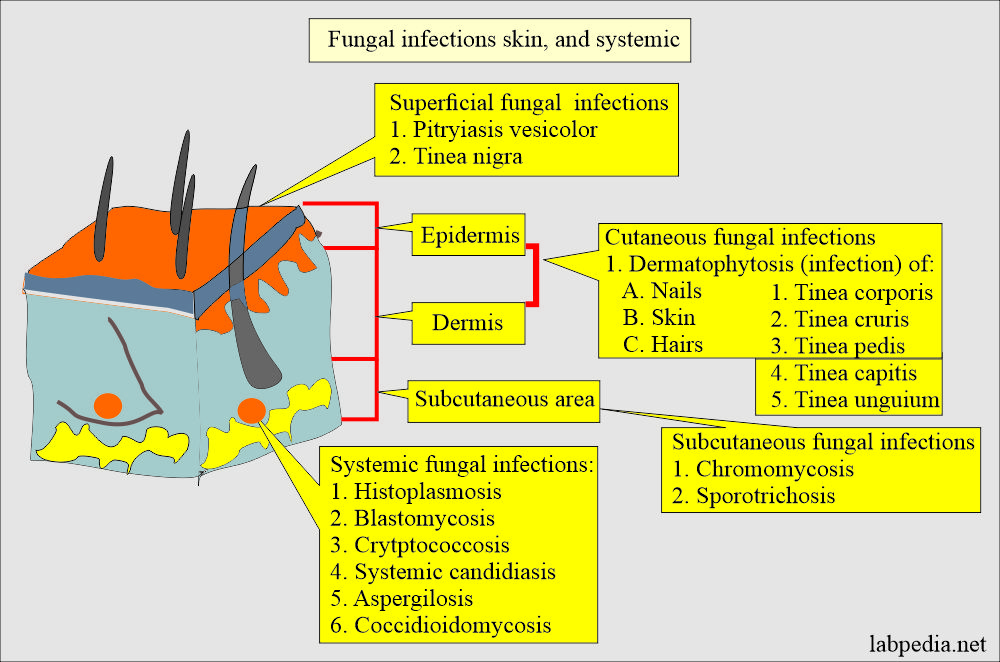
As we can see from the illustration, Black Skin Fungal Skin has many fascinating aspects to explore.
The causes of black skin fungal skin are multifaceted and involve various factors, including:
- Skin Type: People with black skin may be more prone to fungal infections due to their skin's natural pH and moisture levels.
- Humidity: Warm and humid environments can create an ideal environment for fungal growth.
- Exposure: Exposure to certain environments, such as compost, animal dung, or decaying organic matter, can increase the risk of fungal infections.
- Skin Damage: Cuts, scrapes, or burns can create an entry point for fungal spores, leading to infections.
- Immunocompromised Status: People with weakened immune systems, such as those with diabetes, cancer, or taking immunosuppressive medications, are more susceptible to fungal infections.
Diagnosis of Black Skin Fungal Skin
Diagnosing black skin fungal skin requires a thorough examination of the skin and a comprehensive medical history. A doctor may use the following methods to diagnose a fungal infection:

- Skin Scrapings: A doctor may take a skin scraping from the affected area and examine it under a microscope or place it in a culture medium to identify the fungus.
- Cultures: A doctor may take a culture from the affected skin and examine it in a laboratory to identify the fungus.
- Biopsy: In some cases, a doctor may take a biopsy from the affected skin to examine it under a microscope or place it in a culture medium.
Treating black skin fungal skin requires a comprehensive approach that involves both medical and lifestyle changes. A doctor may prescribe the following treatments:
- Antifungal Medications: Topical or oral antifungal medications can help clear up the infection and prevent it from spreading.
- Creams and Ointments: Over-the-counter creams and ointments containing ingredients such as clotrimazole, miconazole, or terbinafine can help treat fungal infections.
- Home Remedies: Apple cider vinegar, tea tree oil, and aloe vera gel can help soothe and calm the skin, reducing the risk of infection.
Prevention of Black Skin Fungal Skin
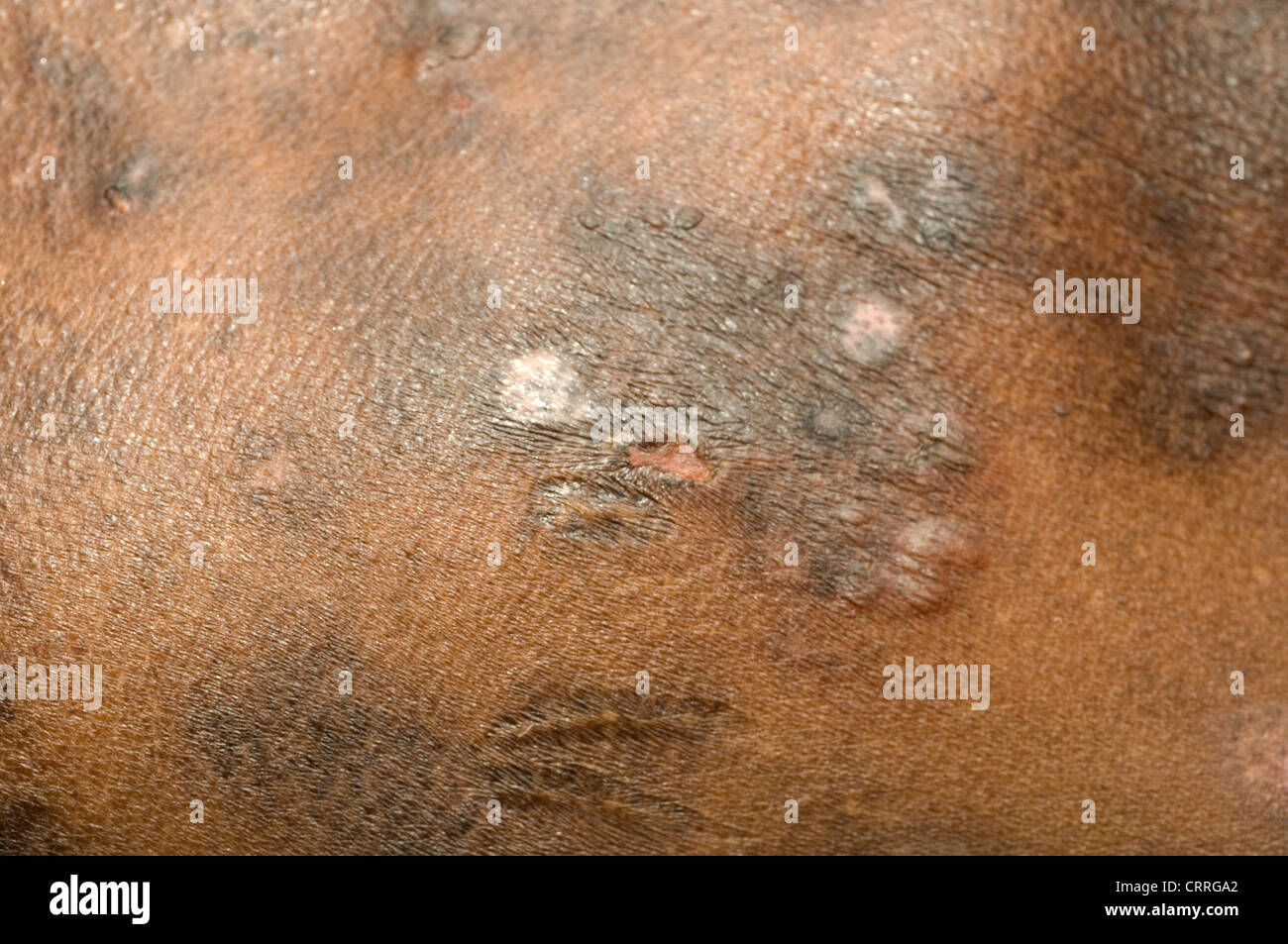
Preventing black skin fungal skin requires maintaining good skin hygiene and avoiding exposure to potentially infected environments. Some tips to prevent fungal infections include:
Conclusion
Black skin fungal skin is a rare but potentially life-threatening fungal infection that requires prompt medical attention. Understanding the causes, diagnosis, and treatment of black skin fungal skin is essential to preventing and treating this condition. By maintaining good skin hygiene, avoiding exposure to potentially infected environments, and following a comprehensive treatment plan, individuals can prevent and treat black skin fungal skin and maintain healthy, clear skin.